
Jun 25, 2019
PRESTIGE AF is a €6.9m project, aimed at patients with atrial fibrillation (AF), a common heart condition which causes irregular and abnormally fast heartbeat, who have previously had a stroke caused by bleeding in the brain (termed intracerebral haemorrhage or ICH). The Prevention of Stroke in intracerebral hemorrhage survivor with Atrial Fibrillation (PRESTIGE-AF) brings together scientists and clinicians across Europe with the goal of reducing the risk of further stroke in this group of patients.
At the core of the PRESTIGE-AF project is a clinical trial to gather evidence around recommended medication for stroke prevention in patients with AF. Several sub-studies will explore individual predictive risk modelling using brain imaging, genetic testing and other biological markers. Other aspects of the project include exploring cognitive and psychological factors and drug adherence by patients.
Congratulations to the team at Imperial College Healthcare NHS Trust (UK) who randomised the first participant into the PRESTIGE-AF Study, while other sites across Europe are underway to do the same.

The team at Imperial College Healthcare NHS Trust who randomised the first participant. From left: Vaishali Dave, Peter Wilding, Ana Gil, Sheila Mashate (front-right). Congratulations to the team!
The Stroke Alliance for Europe (SAFE) has responsibility in the project for disseminating information about TENSION to the stroke community. For more information, please contact research@safestroke.eu.
PRESTIGE-AF has received funding from the European Union’s Horizon 2020 research and innovation programme under grant agreement No 754517.

Jun 21, 2019
“The municipalities (in Norway) govern themselves regarding the economy and the government can’t earmark money to be used in the municipalities for each purpose. The municipal decides what they want to use the money for. And too often we see that there are no more money left when it comes to give patients the treatment they need, and which Norwegian law grants them” says Bjørn Bakke, leader of the Norwegian Stroke Support Organisation, Norsk forening for slagrammede, which is a member of SAFE.
SAFE: What is one issue related to the life after stroke in your country that you think needs special attention?

Photo: Bjørn Bakke, private archive
BB: In Norway we see that the situation for stroke survivors gets worse after the initial treatment in the stroke unit in hospitals and the first rehabilitation in the hospitals. These treatments (medical, surgery, rehabilitation) are financed by the government and follows in most cases national guidelines which are developed and refined during the (last) years. These treatments are usually of a very high quality.
The problem arises when the patient leaves the governmental treatment and the local municipal takes over the rehabilitation. There are of course laws regulating that a patient is granted the same treatment. But unfortunately, this is not necessarily so – in most cases. Norway has approx. 400 municipalities and every single one has a different approach to this issue. To be short, it comes down to economy.
SAFE: What would be the solution, i.e. what is your organisation’s position regarding this issue?
BB: There are 4 stroke organizations in Norway, and we have all concluded that we must engage politicians so that the parliament can pass new laws to strengthen the rights for the patients. This year we have local elections, and this gives us all a great opportunity to address municipal politicians all over Norway. We have a lot of work to do to address the public and the politicians with arguments. This means writing to the politicians and in newspapers and influence the wherever possible, like using Facebook etc.
SAFE: Please tell us more about your organisation.
BB: Our organization is driven by stroke injured people and our main issue is to work for stroke injured people. We are a nonprofit organization having approx. 1250 members spread all over Norway in 19 local organizations. We plan to establish more local organization, but we see also that we need to change our structure a bit in some places. Some of the local organizations cover a too large area and it is not possible for them to gather people from all over their area, so we may need to split some large organizations into smaller units.
Neuropathic Pain After Stroke
Dr Hege Ihle-Hansen, specialist in inner medicine and geriatrics at Oslo University hospital, Ullevål, told us that in follow-up after stroke a neuropathic pain is also mapped, and this is included in the national guidelines concerning follow-up 3 months after stroke.
Grethe Lunde, a stroke survivor, member of Norsk forening for slagrammede and SAFE Board member is one of many stroke survivors who live with neuropathic pain.
“How to live with muscle pain/neurological pain after 25 years as a stroke survivor? Well, I am really happy to be a knitter, as knitting often cuts the link to the “pain button” in our brain. It is a great way to disconnect from what is hurting. Knitting is also great fun and a really good tool for enhancing the mobility in your hands. Knitting distracts you from chronic pain. A study conducted by Harvard Medical School’s Mind and Body Institute, found that knitting lowers heart rate, by an average of 11 beats per minute, and induces an “enhanced state of calm, similar to that of yoga” concluded Grethe.

Photos by: Grethe Lunde Some of the knitting patterns that Grethe knitted recently.


Jun 14, 2019
This week we spoke with leaders of two SAFE member organisations from Ukraine, Prof. Liliya Zviagina, MD, PhD, President of the stroke support organisation ‘Victory over Stroke’ and Dmitriy Gulyayev, MD, PhD, Director of publishing and research projects, Medical adviser of public subdivision, Ukrainian Anti-Stroke Association.
“I would say that in the information related to stroke and stroke care in Ukraine, provided by some specialists and even institutions, there is a lot of inaccuracies, mistakes, and even obvious and impertinent lie and falsifications” said Dmitriy Gulyayev at the very beginning of our conversation.

Dmitriy Gulyayev
SAFE: What is one issue related to the life after stroke in your country that you think needs special attention?
 DG: Current state of stroke care in Ukraine is poor, so it is not easy to pick just one problem. In my opinion, one of the major issues is that special needs of stroke survivors are neglected by the society and the government. Stroke survivors are isolated from public – physically (due to inaccessible public transportation, buildings etc.), and psychologically (as they are often ashamed of their disabilities). They are not in focus and are almost ‘invisible’ for the society. Despite the fact that virtually anyone in Ukraine has a family member or a friend who suffered a stroke, they do not realize how many stroke survivors there are in Ukraine, how challenging their life is, and how unfair the society and the government treat this huge sub-population – stroke survivors, their relatives and caregivers.
DG: Current state of stroke care in Ukraine is poor, so it is not easy to pick just one problem. In my opinion, one of the major issues is that special needs of stroke survivors are neglected by the society and the government. Stroke survivors are isolated from public – physically (due to inaccessible public transportation, buildings etc.), and psychologically (as they are often ashamed of their disabilities). They are not in focus and are almost ‘invisible’ for the society. Despite the fact that virtually anyone in Ukraine has a family member or a friend who suffered a stroke, they do not realize how many stroke survivors there are in Ukraine, how challenging their life is, and how unfair the society and the government treat this huge sub-population – stroke survivors, their relatives and caregivers.
Unfortunately, stroke survivors themselves rarely volunteer to share their experiences and challenges, and thus we are unable figure out the list of their priorities, and often have no other choice than initiating projects at our own discretion. Moreover, stroke survivors are not prepared to join their forces to speak up about their problems and the unmet needs. As a result, official institutions, take care of those who are younger, more mobile, more active, and who are shouting about themselves louder. Particularly by this reason, among others, for example, rather influential social movement “Patients of Ukraine” was established and is managed and promoted by activists of HIV/AIDS and hepatitis organizations, and stroke items are far out of their interest and attention.

Liliya Zviagina
 LZ: Stroke is the leading cause of morbidity and mortality death in Ukraine and is the main cause of disability in adults. Number of sufferers varies from 200 -300 per 100 000 population, depends on region. The main risk factors for stroke are well understood and include atherosclerosis and high blood pressure as well as bad habits. Stroke has a harmful impact on social and family life.
LZ: Stroke is the leading cause of morbidity and mortality death in Ukraine and is the main cause of disability in adults. Number of sufferers varies from 200 -300 per 100 000 population, depends on region. The main risk factors for stroke are well understood and include atherosclerosis and high blood pressure as well as bad habits. Stroke has a harmful impact on social and family life.
Quality of stroke service varies from region to region and depends on sometimes from personal activities and forces of doctors. To promote good service for stroke patients we have understand what is wrong and what we could to do in existing conditions.
Stroke service in Ukraine is only in the beginning of the way, people could not always access the services they need. I would like to stress on some common problems in Ukraine and what changed during last years.
1/ People are not aware about stroke;
2/ Not all people address in time to get help;
3/ Not enough stroke units;
4/ There are not insurance, and patients must pay for their treatment;
4/ Stroke patients get treatment in general neurological department
5/ Not so many departments use modern treatment (thrombolytic therapy and thrombectomy);
6/Not so many departments are equipped for monitoring vital parameters of stroke patients;
7/ Not so many departments have trained staff to perform all needs of stroke patients, particularly who has a dill with sufferers who have communications problems caused by stroke, such as aphasia;
8/ Not so many departments have multidisciplinary teams;
9/ Early and later rehabilitation are poorly organized;
10/ Not all stroke survivors and their carers are provided with the recommendation they need when they discharge from the hospital;
11/There are not system for observe patient during the first year;
12/ Not all patients are offered individual budgets or direct payments within the first six weeks of their returning home;
13 Not all people has a good knowledge of primary and secondary stroke prophylactic
SAFE: What would be the solution, i.e. what is your organisation’s position regarding this issue?
DG: Obviously, there is no magic wand to solve this deep social problem. We have to be ready for long-lasting, often thankless routine activities. We have to:
-widely distribute through different channels stories about stroke survivors’ life, needs, problems, solutions – not only in Ukraine, but in other countries with different level of social and economic development;
-build different platforms (both real and virtual) for communication of stroke survivors – peer-to-peer, and with surrounding world;
-involve stroke survivors into elaboration of stroke care on national, regional and local levels, encourage their active self-advocacy.
LZ: This can be summarized in couple of points:
1. The ministry of health declares some prevention measures; there is program -“Available medications”, which covered costs anti-hypertensive medicine, medicine to treat diabetes, …
2. The ministry of health proved protocol of ischemic stroke treatment N602 from 03/08/2012 which is act till now, should be revised according new trends, including thrombectomy
Over the last years the number of stroke units and thrombolytic therapy increased considerably as well as clinic where clot retrieving is available.
Despite of it we must improve these directions, which are help not only survive but return to social life.
SAFE: Please tell us more about your organisation
DG: The Ukrainian Anti-Stroke Association (UASA) is the All-Ukrainian nongovernmental organization established in 2004 with the purpose of integrating efforts of medical professionals, scientists, teaching staff of medical educational institutions, workers of social services, mass-media and people at large for improving the health care system in treating patients with stroke, primary and secondary stroke prevention, rehabilitation of patients after stroke and improving quality of medical and social help for patients who had stroke. Since its establishment, UASA is one of the most aggressively working Ukrainian NGOs in the field of medicine and health care, and the single organization totally devoted to stroke.
UASA elaborates, publishes and disseminates National Guidelines on stroke care, holds the most important Ukrainian scientific and education events for stroke physicians and allied health care professional, publishes as its official printed matter the single Ukrainian professional journal totally devoted to stroke “Sudynni Zakhvoryuvannya Golovnogo Mozku” (Cerebrovascular Diseases). For 4 years (2010-2013) UASA was publishing the Russian-language version of the “International Journal of Stroke” – the official printed matter of the World Stroke Organization – for all countries where Russian language is in use, including Russia. Several years ago, UASA has initiated and since then is a leader in the SUNEP – stroke unite nurses education project, which is very useful and successful not only in Ukraine, but in other countries of Eastern and Central Europe.
Main directions of work with general population are educational events for stroke survivors and their caregivers, educational materials for patients and general population, particularly the brochures on different aspects of stroke, “Guidebook on neurological diseases for laymen”, etc. The book “Stroke: Information for those who are concerned” has been re-published 8 times.
We fulfil wide educational activity in Facebook, and currently are on the way to finalize and publish the popular web-resource on stroke for general audience. UASA always was the principal organizer of the activities related to the World Stroke Day in Ukraine.
UASA is member of World Stroke Association and European Stroke Organization and is on the final stage of joining SAFE.
LZ: School for stroke survivors “Victory over stroke” was establish within Odessa neurological society in 2008, after visiting SAFE conference. We started with a small group of stroke survivors, trying to manage their life better, arranging some musical concerts, meetings and courses. We work and people help us as a volunteer. Since 2013 I become general neurologist of Odessa health department and from this time, I try to change the system of patient’s service and act more globally. We are working on many directions:
1.People information, (TV, meetings, newspapers)
2.Stroke prevention (patients and doctors)
3.We are involved in city program “Health” which let our patients get access to CT in acute stage for free and get three days treatment according to protocol, this year we have plane to open three stroke units (one is ready now)
4.Thrombolytic therapy will be paid by this program as well as thrombus retrieving.
5.There two telemedicine centers, where patients from the countryside have access for consultations
6.We teach doctors, mange local, national and international conferences.
7.Late rehabilitation center was open in one of Odessa clinic, where patients have accesses to improve their motor dysfunction, be adapt to the city and home environment
8.I joined school to University of third age, where people improved social life to study a lot of new subjects, computers, languages, tourist’s routes, where I teach people different medical questions, presented brochures, given to our organisation by SAFE, and presented new directions of stroke treatment, etc. This kind of activity play positive role, students of the university recognized stroke in one of the visitors and give help him immediately
9.Mortality after ischemic and haemorrhagic stroke decreased
Photo credits: Facebook (Roman Shwed, featured photo); profile photos of the interviewed persons: Personal archive

Jun 13, 2019
SAFE member organisations from Eastern and Central European cluster gathered on 12th June in Krakow, Poland to discuss the following items:
- A review of SAFE’s work, including the updating of its strategy and a discussion of its relationship with, and activities addressing the importance of co-morbidities
- Discussion of the implementation of the Stroke Action Plan for Europe, focusing particularly on work that can be done in each country and stakeholder engagement and partnership in advocacy
- An update on the Romanian Presidency event
- Translations of materials and promotion of the prevention website
- Utilisation of the SSOFT website to enable growth of SSOs and more effective advocacy
- Preliminary findings and messages arising from the Economic Impact of Stroke research
- SAFE Research Projects
- SAFE and World Stroke Day 2019
- MERZ Spasticity project
- Round-up of activity from attending members
SAFE is thankful to Boehringer Ingelheim for the continued sponsorship of our Regional Conferences.

Jun 10, 2019
 At the occasion of the 30th Anniversary of the Summer Stroke School in Dubrovnik, Croatia, the Croatian Academy of Sciences, Department of Medical Sciences published a book “Healthy Lifestyle and Prevention of Stroke and Other Brain Impairments”. SAFE Board member, Prof. Anita Arsovska from North Macedonia, contributed to this book with information about SAFE and our political activities.
At the occasion of the 30th Anniversary of the Summer Stroke School in Dubrovnik, Croatia, the Croatian Academy of Sciences, Department of Medical Sciences published a book “Healthy Lifestyle and Prevention of Stroke and Other Brain Impairments”. SAFE Board member, Prof. Anita Arsovska from North Macedonia, contributed to this book with information about SAFE and our political activities.
30th Dubrovnik Summer Stroke School: Healthy Lifestyle and Prevention of Stroke and Other Brain Impairments, International Course, endorsed by European Stroke Organization (ESO), World Stroke Organization (WSO), European Academy of Neurology (EAN) and World Federation of Neurology (WFN) took place in Dubrovnik, Croatia, at the Inter-University Center, from 3-7th of June 2019.
The scientific programme was exciting and encompassed many aspects of stroke and related disorders (starting from prevention, acute diagnosis, treatment and rehabilitation) delivered by international faculty from Albania, Austria, Croatia, Germany, Israel, N. Macedonia, Serbia and Slovenia. Traditionally, the school was attended by numerous participants (residents and young specialists in Neurology) from Albania, Austria, Bosnia and Herzegovina, Croatia, North Macedonia, Serbia and the Netherlands.
“The Voice of the Stroke Survivor Represented Through Stroke Alliance for Europe” was delivered by Prof. Anita Arsovska (N. Macedonia), SAFE Board Member, with a special focus on the European Stroke Action Plan 2018-2030 and the most important overarching targets that need to be fulfilled by 2030.
Further on, the political activities of SAFE were presented, such as regular Stroke Summits in the European Parliament and the European Commission of the Regions in Brussels, as well as the importance of collaboration with other societies and initiatives (such as ESO, Angels Initiative, WSO etc).
SAFE would like to thank our Croatian colleagues from Hrvatsko društvo za prevenciju moždanog udara, our member organisation, for their support and for enabling this promotion of SAFE’s activities.

Prof. Vida Demarin with faculty and participants of the 30th Summer Stroke School in Dubrovnik 2019.
About 30th Dubrovnik Summer Stroke School
Course Director was Prof. dr. Vida Demarin, FAAN, FAHA, FESO, FEAN, FWSO, Fellow of Croatian Academy of Sciences and Arts, University of Zagreb, Croatia and the Board of Directors consisted of Prof. dr. Roman Haberl, University of Munich, Germany, Prof. dr. Kurt Niederkorn, University of Graz, Austria, Prof. dr. David Russell, Univeristy of Oslo, Norway and Assist. prof. dr. Hrvoje Budinčević, Sveti Duh University Hospital, Zagreb. Colleagues from the Dubrovnik General Hospital participated in the Organizing Committee (Dr Andrijana Bogoje Raspopović, Assist. Prof. dr. Denis Čerimagić, Dr Mira Ivanković and Dr Maro Vodopić) and also served as Course Coordinators (Dr Andrijana Bogoje Raspopović, Dr. Petra Črnac Žuna and Petra Dalić). The Summer Stroke School was organized by the International Institute for Brain Health, Central and Eastern European Stroke Society, Croatian Stroke Society, School of Medicine, University Of Zagreb, Inter University Centre Dubrovnik, WFN Applied Research Group on the Organisation and Delivery of Care and the Society for Neuropsychiatry and co-organized by the Department of Medical Sciences – Croatian Academy of Sciences and Arts.
The 30th Summer Stroke School was accredited by 4 ECTS points and provided an excellent and enjoyable platform to hear great lectures, interact with faculty, share experience and meet colleagues from different countries.

Jun 7, 2019
 “When patients after stroke meet and can get together with others – even with non-stroke-patients, their self confidence grows, they start to connect with people, and that is for us very important” says Alžbeta Husarovič, the President of the Slovakian Stroke Support Organisation Porážka.sk and a stroke survivor.
“When patients after stroke meet and can get together with others – even with non-stroke-patients, their self confidence grows, they start to connect with people, and that is for us very important” says Alžbeta Husarovič, the President of the Slovakian Stroke Support Organisation Porážka.sk and a stroke survivor.
SAFE: What is one issue related to the life after stroke in your country that you think needs special attention?
AH: If we have to choose only one issue, it would probably be the socialization. Because with socialization starts all the patient´s effort to ´start over´ and to be able to get back to his previous life as much as it is possible. We believe, that step by step this might be the key to the mental recovery, which is as important as the physical one.
SAFE: What would be the solution, i.e. what is your organisation’s position regarding this issue?
AH: During the last couple months, we at our organisation Porážka.sk are focusing on different activities, which might be helpful to stroke survivors.
We believe that one of those is our Charity run (called Beh neporazených) which unites the patients with healthy people, who are running to raise money and create better conditions for patients. This is the most powerful (but also emotional) project of our organization so far, where the socialization of stroke survivors is really visible. Other our project is focusing on small sheltered workshop, where the patients with disability becoming a real paid work. Sheltered workshop is going to be a place where again patients are exposed to real life and can communicate and bond with others.
SAFE: Please tell us more about your organisation.
AH: Our association Porážka.sk was created in 2013 by Alžbeta Husarovič, stroke survivor. We have three important activities.
- We are trying to spread stroke awareness by organizing various public events such as Unbeaten RUN, Fashion Show etc where we always invite stroke survivors, famous faces and media people.
- We help individuals, stroke survivors and their families in three ways. Financially, by lending to survivors physiotherapeutical equipment and guide them after leaving hospital.
- We are going to give to stroke survivors a place, where they can meet, talk, compare each other, rehabilitate and what is the most important, we are going to give them a work.
Photo credits: Porazka.sk Facebook page.

Jun 6, 2019
“European Obesity Day celebrated every May, brings people together to raise awareness and increase knowledge about obesity and the many other diseases on which it impacts. The aim is to get coordinated action to improve the prevention and treatment of obesity and ultimately to improve the health and quality of life of those who are living with it. The causes of obesity and overweight are known whereby there is an energy imbalance between calories consumed and calories expended. This is being fueled by an increased intake of energy-dense foods that are high in fat, sugar and salt and an increase in physical inactivity due to the increasingly sedentary nature of many forms of work, changing modes of transportation, and increasing urbanisation. Obesity is a disease often caused by factors largely beyond an individual’s control. It is a highly complex matter whereby changes in dietary and physical activity patterns are often the result of environmental and societal changes associated with development and lack of supportive policies in sectors such as health, agriculture, transport, urban planning, environment, food processing, distribution, marketing and education” said Dr Charmaine Gauci, Superintendent of Public Health, Ministry for Health, Malta.
In the meantime, SAFE is focused on what we could do as individuals to tackle this problem and reduce chances of getting a stroke. In Europe, 51.6% of adults are overweight. Being obese not only increases your risk of high blood pressure, heart disease and diabetes, but also makes you more likely to have a stroke, particularly if you are carrying extra weight around your stomach. Fortunately, this is yet another risk factor that can be potentially altered through a healthy diet, exercise and other lifestyle changes.
The relationship between abdominal obesity and stroke is long established, particularly where other conditions are also present, such as diabetes, high blood pressure and high cholesterol. But there are different opinions as to why the risk is increased in overweight people.
Some studies suggest body mass index (BMI) alone is not a good indicator for stroke risk. Instead, researchers claim excess stomach weight may be a stronger predictor. A waist measurement of over 40 inches in men and over 35 inches in women is classed as abdominal obesity.
If you wish to know more about obesity and stroke, and, more importantly, what you could do to decrease the risk of stroke, please visit our website www.strokeprevention.info for more information.
Jun 4, 2019
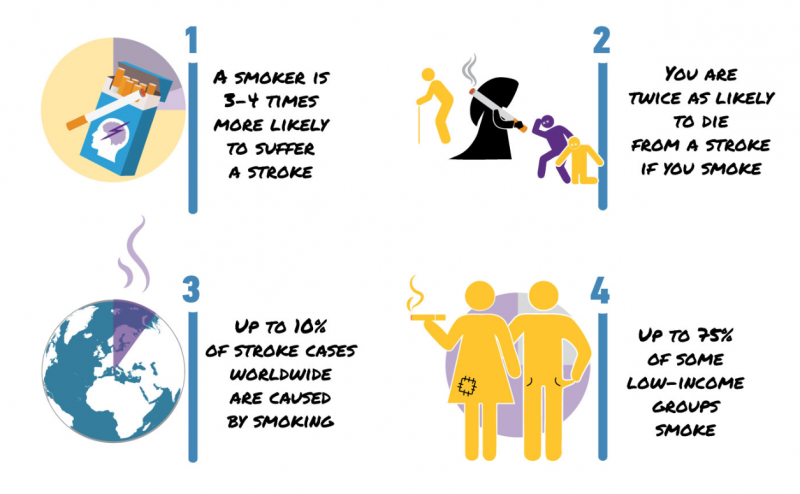
Each 31 May, the World No Tobacco Day is being celebrated around the globe by raising awareness about the harmful and deadly effects of smoking and the use of tobacco products. SAFE is trying to raise awareness about the dangers of smoking for another very important reason- Smoking is one of the modifiable stroke risk factors. Many studies suggest smoking almost doubles the risk of stroke and subarachnoid haemorrhage (SAH), a life-threatening type of stroke caused by bleeding into the space surrounding the brain (1). Long-term exposure to nicotine has many negative health effects. Some, such as a persistent cough, are noticeable. Whereas the hidden damage that happens within the brain is not often apparent until it’s too late. Research shows that the parts of a smoker’s brain that control everyday tasks, such as hand-to-eye coordination, are reduced in volume, which can impair its function (2).
According to the Statement given by EU Commissioner for Health and Food Safety, Vytenis Andriukaitis, on a global level, the figures are staggering – there are more than 7 million tobacco-associated deaths around the world each year. This is one of the main reasons why the EU and its Member States are active supporters of a global health treaty – the Framework Convention on Tobacco Control of the World Health Organisation.
“Tobacco consumption is the single largest avoidable health risk, and the most significant cause of premature death in the EU, responsible for nearly 700,000 deaths annually. This is not just a dry number. These are our family members, friends, colleagues. I am particularly concerned about young people taking up vaping and various new products like heated tobacco products and e-cigarettes, which are increasingly being marketed with misleading claims. 29% of young Europeans aged 15-24 are smoking. How many are using alternatives damaging their young lungs?” asked Mr Andriukaitis.
Up to 10% of stroke cases worldwide are caused by smoking
According to the World Health Organisation, smoking is thought to cause around 10% of cardiovascular disease worldwide. In 2008, the highest overall prevalence for smoking was estimated to be in the European Region, at nearly 29%. (3) Thankfully, in Europe, the death rate has fallen significantly over the last two years, but the number of people living with disabilities, as a result of stroke, continues to be a huge problem (4).
“The EU is working hard to protect citizens from the hazardous effects of tobacco use. One of our key milestone measures in the EU’s fight against illicit trade in tobacco products – the European systems of tobacco traceability and security features – became operational on 20 May. This means that consumers will soon see new traceability markings on the packs, together with the required security features. The traceability markings will enable national authorities to track and trace the movements of tobacco packs across the legal supply chain in the EU. In addition, security features will enable public authorities and citizens to determine if a tobacco product on the market is genuine or illicit” said Mr Andriukaitis in his official statement.
In conclusion, we all know smoking is bad for us. It’s been linked with all kinds of diseases, including stroke. But sometimes even the cold hard facts aren’t enough to make us want to kick the habit. If you’re considering cutting down or giving up, please visit SAFE’s website www.strokeprevention.info dedicated to education about stroke risk factors and check out five tips for quitting smoking.
References:
- James F. Meschia, MD et al. (2014). Guidelines for the Primary Prevention of Stroke. A statement for healthcare professionals from the American Heart Association/American Stroke Association. DOI: 10.1161/STR.0000000000000046. Stroke, 45: 3754-3832.
- Lim, T. S., Lee, J. S., Yoon, J. H., Moon, S. Y., Joo, I. S., Huh, K., & Hong, J. M. (2017). Cigarette smoking is an independent risk factor for post-stroke delirium. BMC neurology, 17(1), 56.
- Thun MJ, Apicella LF, Henley SJ. (2000). Smoking vs other risk factors as the cause of smoking-attributable deaths: confounding in the courtroom. JAMA, 284:706–712
- https://www.stroke.org.uk/sites/default/files/the_burden_of_stroke_in_europe_-_challenges_for_policy_makers.pdf

Jun 3, 2019
Written by Tom Balchin | First published on https://arni.uk.com
Stroke is one of many conditions that can lead to seizures, or epilepsy. You may think of these as ‘having fits’. In the UK this condition affects just under 1% of the population. Around 5% of people who have a stroke will have a seizure within the following few weeks. These are known as acute or onset seizures and normally happen within 24 hours of the stroke.
The good news is that your risk of having a seizure lessens with time following your stroke. But, you’ve really got to take care. I see people regularly who have fits for the first time. It’s never fun, but luckily, as someone who has had controlled epilepsy for over 20 years I know exactly how to identify these very early (it’s not that hard really). Quickly get the person to the floor, gently, into the recovery position and call for an ambulance. If you have a list of all their medications on hand to tell the paramedic, that would be ideal.
You are more likely to have had one if you have had a severe stroke, a haemorrhagic stroke or a stroke involving the part of the brain called the cerebral cortex. My own epilepsy came only after subarachnoid haemorrhage, (an uncommon, very serious and often fatal type of stroke caused by bleeding on the surface of the brain)
The causes of seizures are complex. Cells in the brain communicate with one another and with our muscles by passing electrical signals along nerve fibres. If you have epilepsy this electrical activity can become disordered and a sudden abnormal burst of electrical activity in the brain can lead to a seizure.
There are over 40 different types of seizures that can occur, but the most common ones are partial seizures or generalised seizures.
Partial or focal seizures only occurs in part of your brain. You may remain conscious and aware of your surroundings during a partial seizure (called a simple partial seizure) or you may become confused and unable to respond (a complex partial seizure). The symptoms you experience during a partial seizure will depend on which part of your brain has been affected. You may feel changes in sensation such as a tingling feeling, which spreads to other parts of your body.
Commonly people experience a rising feeling in their stomach (a bit like when you go over a humpback bridge). This is called an ‘epigastric rising sensation’. You may also experience uncontrollable stiffness, twitching or turning sensation in a part of the body such as your arm or hand, and/or disturbances in your vision, such as seeing flashing lights.
You can read the full article here.
Image credits: Pixabay.com

May 31, 2019
The European Chronic Disease Alliance (ECDA), the European Public Health Alliance (EPHA) and the NCD Alliance publish the paper “Towards an EU-Strategic Framework for the Prevention of Non-communicable Diseases” concluding that a new EU strategic framework to prevent non-communicable diseases (NCDs) is needed to address chronic diseases, the 21st century’s foremost health threat.
With 70% of respondents to a recent EU Barometer survey wanting to see more EU action on health and with epidemic levels of NCDs undermining people’s well-being, healthcare systems, and Europe’s economic and social prosperity, preventing NCDs should be a main priority for the next European Commission.
The mandate 2019-2024 is an opportunity to act upon commitments made at the UN High Level Meeting on NCDs in September 2018 and follow on the EU Reflection Process on Chronic Diseases to deliver concrete solutions to respond to the main common risk factors. While progress is made on reducing premature mortality from NCDs, longer lives do not necessarily translate into healthy lives.
With stroke being such an important topic among other non-communicable diseases, SAFE and ESO recently organised a panel discussion in the Committee of Regions in Brussels, under the Patronage of The Romanian Presidency, exploring the role of policy in tackling stroke. During the panel discussion, patient representatives and clinical experts called on the EU Institutions to recognize the burden of stroke as its own incredibly important entity, rather than diluting it in the wider classification of cardiovascular diseases. Panelists representing patients and clinicians also called for the EU to facilitate discussions between its Member States on the implementation of the Stroke Action Plan for Europe. As a next step to this meeting, SAFE and ESO begun a follow-up with speakers and participants to move forward with the identified opportunities. The immediate action that came as a result of this panel discussion was SAFE’s participation in the CHRODIS+ Conference, held in Budapest, Hungary on 15 May 2019. At this important meeting, SAFE was represented by Grethe Lunde, SAFE Board Member and a stroke survivor from Norway. SAFE actively participated in discussions on topics such as patient involvement, multi-morbidity, integrated care and employment.
Europeans spend between a quarter and a fifth of their lives in ill-health. 700 billion EUR is spent on treating NCDs in the EU each year – although many chronic diseases are to a considerable degree preventable. The paper proposes basic principles, priorities and actions for such an EU strategic framework, setting out a roadmap to make change happen. For more information, please contact: info@alliancechronicdiseases.org or epha@epha.org.









 DG: Current state of stroke care in Ukraine is poor, so it is not easy to pick just one problem. In my opinion, one of the major issues is that special needs of stroke survivors are neglected by the society and the government. Stroke survivors are isolated from public – physically (due to inaccessible public transportation, buildings etc.), and psychologically (as they are often ashamed of their disabilities). They are not in focus and are almost ‘invisible’ for the society. Despite the fact that virtually anyone in Ukraine has a family member or a friend who suffered a stroke, they do not realize how many stroke survivors there are in Ukraine, how challenging their life is, and how unfair the society and the government treat this huge sub-population – stroke survivors, their relatives and caregivers.
DG: Current state of stroke care in Ukraine is poor, so it is not easy to pick just one problem. In my opinion, one of the major issues is that special needs of stroke survivors are neglected by the society and the government. Stroke survivors are isolated from public – physically (due to inaccessible public transportation, buildings etc.), and psychologically (as they are often ashamed of their disabilities). They are not in focus and are almost ‘invisible’ for the society. Despite the fact that virtually anyone in Ukraine has a family member or a friend who suffered a stroke, they do not realize how many stroke survivors there are in Ukraine, how challenging their life is, and how unfair the society and the government treat this huge sub-population – stroke survivors, their relatives and caregivers.
 LZ: Stroke is the leading cause of morbidity and mortality death in Ukraine and is the main cause of disability in adults. Number of sufferers varies from 200 -300 per 100 000 population, depends on region. The main risk factors for stroke are well understood and include atherosclerosis and high blood pressure as well as bad habits. Stroke has a harmful impact on social and family life.
LZ: Stroke is the leading cause of morbidity and mortality death in Ukraine and is the main cause of disability in adults. Number of sufferers varies from 200 -300 per 100 000 population, depends on region. The main risk factors for stroke are well understood and include atherosclerosis and high blood pressure as well as bad habits. Stroke has a harmful impact on social and family life.

 At the occasion of the 30th Anniversary of the Summer Stroke School in Dubrovnik, Croatia, the Croatian Academy of Sciences, Department of Medical Sciences published a book “Healthy Lifestyle and Prevention of Stroke and Other Brain Impairments”. SAFE Board member, Prof. Anita Arsovska from North Macedonia, contributed to this book with information about SAFE and our political activities.
At the occasion of the 30th Anniversary of the Summer Stroke School in Dubrovnik, Croatia, the Croatian Academy of Sciences, Department of Medical Sciences published a book “Healthy Lifestyle and Prevention of Stroke and Other Brain Impairments”. SAFE Board member, Prof. Anita Arsovska from North Macedonia, contributed to this book with information about SAFE and our political activities.

 “When patients after stroke meet and can get together with others – even with non-stroke-patients, their self confidence grows, they start to connect with people, and that is for us very important” says Alžbeta Husarovič, the President of the Slovakian Stroke Support Organisation Porážka.sk and a stroke survivor.
“When patients after stroke meet and can get together with others – even with non-stroke-patients, their self confidence grows, they start to connect with people, and that is for us very important” says Alžbeta Husarovič, the President of the Slovakian Stroke Support Organisation Porážka.sk and a stroke survivor.






