
Jan 15, 2020
We are delighted to share with you a report from the German Stroke Foundation about their key activities between July and December 2019. We hope it will inspire you and your organisation for activities in your country.
World stroke day: “Every step counts”

Miriam_Mashkoori, World Stroke Day 2019
Statistically 25 percent of the worlds population gets a stroke. This also means: 3 out of 4 people do not get a stoke!
Around World Stroke Day (October 29th) the German Stroke Foundation raised awareness for stroke-prevention with the slogan “every step counts”. Many papers published the press release with tips for a healthier lifestyle, radio-stations aired an interview with the foundations prevention-expert Miriam Mashkoori. On Facebook people explained how they lost weight or managed to quit smoking to motivate other Facebook-users to live a healthier life.
Summer Camp for children and their families
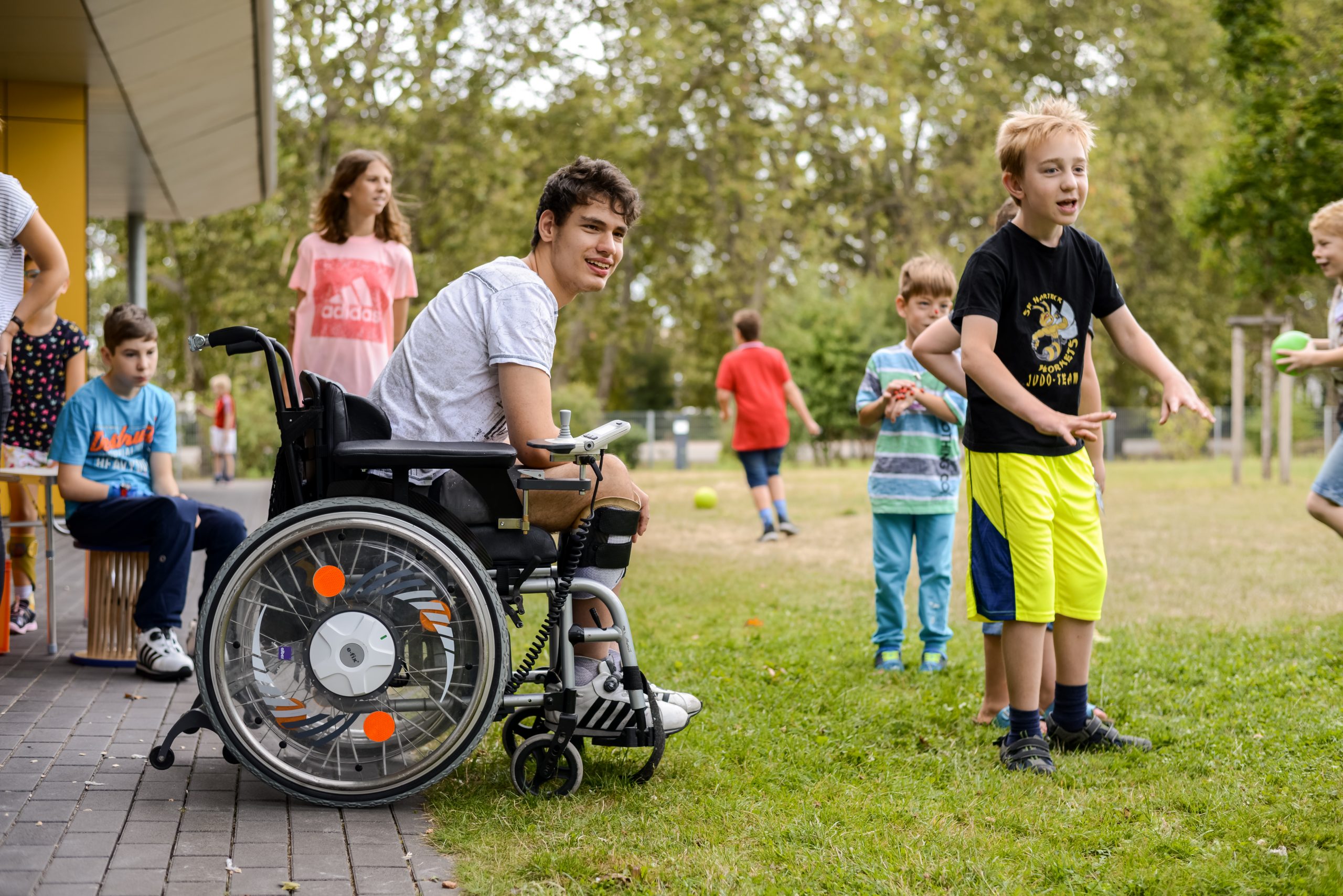 How will my child develop? How will it do in Kindergarten or school? How do we cope with social challenges and which therapies are best with for our child? The diagnosis “stroke” raises many questions – especially when a child is affected. The three day “Summer Camp” offered families with a child affected by stroke an opportunity for an informative and fun-filled weekend. Experts answered questions, psychologists helped developing new perspectives, singer Patricia Kelly gave an exclusive concert and former world-class Wrestler Alexander Leipold offered sport-activities for the children.
How will my child develop? How will it do in Kindergarten or school? How do we cope with social challenges and which therapies are best with for our child? The diagnosis “stroke” raises many questions – especially when a child is affected. The three day “Summer Camp” offered families with a child affected by stroke an opportunity for an informative and fun-filled weekend. Experts answered questions, psychologists helped developing new perspectives, singer Patricia Kelly gave an exclusive concert and former world-class Wrestler Alexander Leipold offered sport-activities for the children.
Tea Time with Liz Mohn
The foundation´s president and founder Liz Mohn invited stroke survivors and supporters of the foundation for a Tea Time. She met and spent a wonderful afternoon with people who were especially engaged in our foundation´s activities.
Workshop for young stroke-survivors
 A stroke affects every aspect of life. Young survivors are even in a special situation. They want to return to work, build or maintain relationships and live an independent life – which is not always possible. In a four-day workshop they had the opportunity to talk to psychologists and doctors and to exchange their own experiences. Word-class Mountainbiker Peter Schermann talked about his return into sports after his stroke.
A stroke affects every aspect of life. Young survivors are even in a special situation. They want to return to work, build or maintain relationships and live an independent life – which is not always possible. In a four-day workshop they had the opportunity to talk to psychologists and doctors and to exchange their own experiences. Word-class Mountainbiker Peter Schermann talked about his return into sports after his stroke.
Public talk about reintegration in working life

After an accident or an illness it is often hard to return to work. Some might not be able to work full hours anymore, others might have to find a completely different job. A staff member of the employment office, an integration expert and a coach for job applications informed about opportunities to get back to work at the event “Forum Schlaganfall (Stroke Forum)” at the German Stroke Foundation in Gütersloh.
Politican Andrea Milz visits the Stroke Foundation
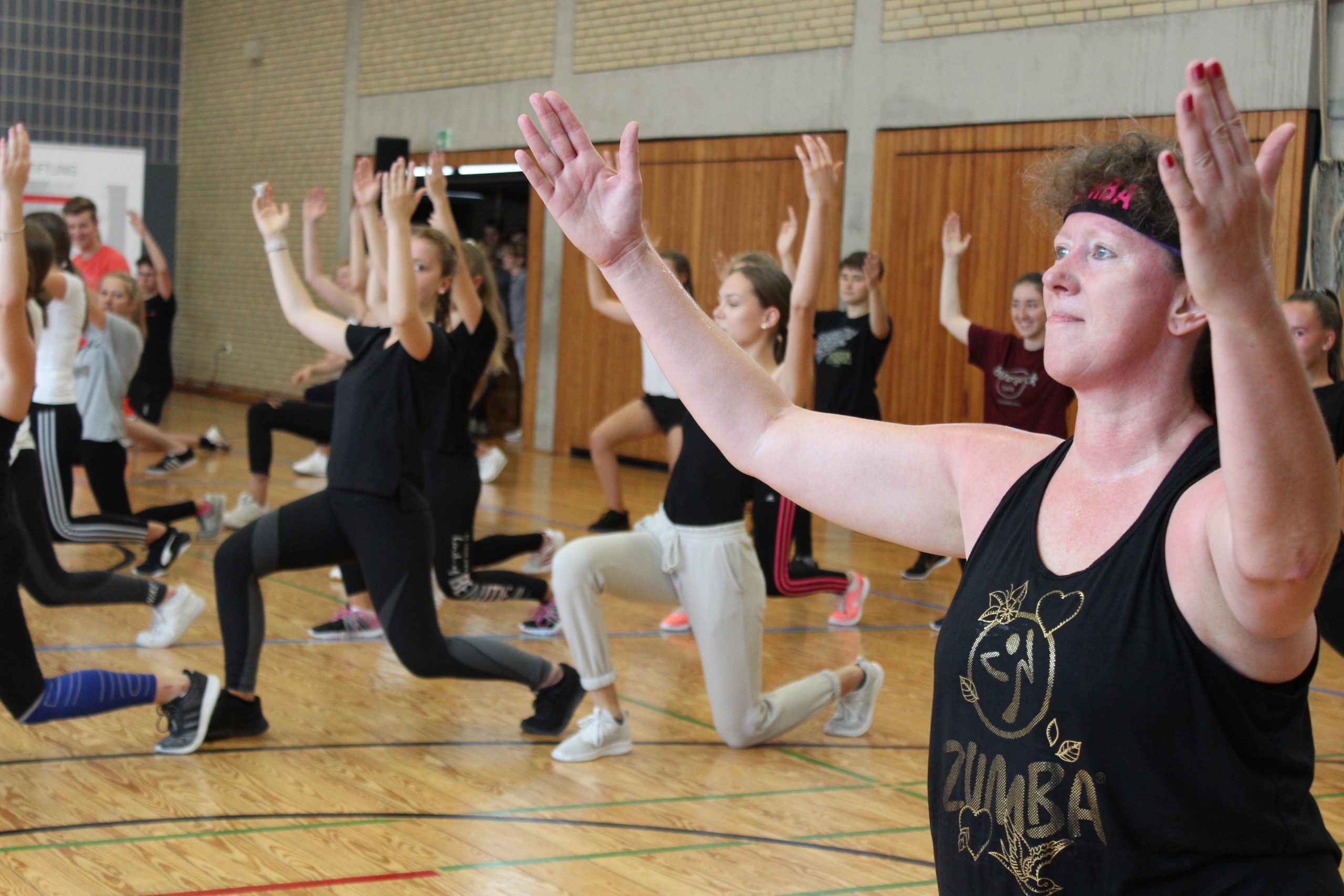
Andrea Milz
The North Rhine Westphalian secretary of state for sports and volunteering, Andrea Milz, visited the German Stroke Foundation to talk about the volunteer-project “stroke helpers”.
As a certified Zumba-trainer she also gave a Zumba-lesson at the local High School. The High School offers optional medicine-classes for its students and cooperates with the foundation.
Speakers of self support groups meet
Speakers of self support groups do not only organise meetings and events for their groups. But they also need to know about relevant changes in law, new therapies or other important aspects about stroke. This is why the foundation offers workshops for speakers of self support groups all over Germany.

Cooperation with TV-show “Unter uns” ends

Patrick Müller
One of the main characters in the popular TV series “Unter uns” has had a stroke in one of the episodes in May. According to the storyboard lawyer Tobias, played by actor Patrick Müller, suffered from hemiplegia and severe speech problems. The team and cast of “Unter uns” cooperated with the German Stroke Foundation in order to create a realistic storyline. The cooperation know officially ended. The fan-club donated more than 1400 Euros for the foundation.
Experts meet to learn about stroke in children
 Not many people know that children can have a stroke. Even experts like podiatrists or therapists often don’t have sufficient information about the topic. The German Stroke Foundation wants to change this by inviting experts to learn more about child stroke. More than 40 doctors and other experts met in Bavaria in 2019.
Not many people know that children can have a stroke. Even experts like podiatrists or therapists often don’t have sufficient information about the topic. The German Stroke Foundation wants to change this by inviting experts to learn more about child stroke. More than 40 doctors and other experts met in Bavaria in 2019.
Photos: German Stroke Foundation, 2019

Jan 10, 2020
First published on ScienceDaily.com
Middle-aged adults with high blood pressure, Type 2 diabetes, heart disease or stroke could be at high risk for cancer and early death when sleeping less than six hours per day, according to new research published in the Journal of the American Heart Association, the open access journal of the American Heart Association.
“Our study suggests that achieving normal sleep may be protective for some people with these health conditions and risks,” said lead study author Julio Fernandez-Mendoza, Ph.D., associate professor at Pennsylvania State College of Medicine and sleep psychologist at the Sleep Research & Treatment Center of the Penn State Health Milton S. Hershey Medical Center in Hershey, Pennsylvania. “However, further research is needed to examine whether improving and increasing sleep through medical or behavioral therapies can reduce risk of early death.”
Researchers analyzed data of more than 1,600 adults (20 to 74 years old, more than half women) from the Penn State Adult Cohort who were categorized into two groups as having stage 2 high blood pressure or Type 2 diabetes and having heart disease or stroke. Participants were studied in the sleep laboratory (1991-1998) for one night and then researchers tracked their cause of death up to the end of 2016.
Researchers found:
Of the 512 people who passed away, one-third died of heart disease or stroke and one-fourth died due to cancer.
People who had high blood pressure or diabetes and slept less than 6 hours had twice the increased risk of dying from heart disease or stroke.
People who had heart disease or stroke and slept less than 6 hours had three times the increased risk of dying from cancer.
The increased risk of early death for people with high blood pressure or diabetes was negligible if they slept for more than 6 hours.
You can read the full article here.
Image: Pixabay.com

Jan 7, 2020
First published on ScienceDaily.com
A team of New Jersey stroke researchers has linked recovery of reading and language competence with cerebral blood flow in the left reading network. Their findings may contribute to new approaches to identifying and treating reading deficits after stroke. The open access article, “Cerebral perfusion of the left reading network predicts recovery of reading in subacute to chronic stroke” was epublished on August 26, 2019 in Human Brain Mapping. The authors are Olga Boukrina, PhD, and A.M. Barrett, MD, of Kessler Foundation, and William Graves, PhD, of Rutgers, the State University of New Jersey.
Despite the fundamental role of reading ability in everyday living, little research has been conducted on patterns of reading recovery after stroke, or the development of interventions to improve reading outcomes. In this study of left-brain stroke, a team of New Jersey scientists examined patterns of cerebral perfusion bilaterally, including left and right networks of brain areas important for healthy reading, the area surrounding the stroke lesion, and the corresponding contralateral area.
They enrolled 31 participants during inpatient rehabilitation, within 5 weeks of left-sided stroke. All underwent functional magnetic resonance imaging, psychometric testing, neurological examination and tests for phonological, orthographic and semantic impairments. Fifteen participants had follow-up studies at 3 months post stroke. Analysis of data from the subacute and chronic phases showed that recovery of reading and language competence correlated with increases in cerebral blood flow in the left reading network.
You can read the full article here.
Image: Pixabay.com

Jan 6, 2020
Source: European Journal of Arrhythmia & Electrophysiology. 2019;5(2):77–81
Authors: Kamal Kishor , Devendra Bisht , Sanjay Kalra
Abstract
Atrial fibrillation (AF) is one of the major causes of stroke, heart failure, sudden death and cardiovascular morbidity in the world. Management of AF, its risk factors and complications demands huge cost. The frequent hospitalisations, haemodynamic abnormalities, and thromboembolic events related to AF put a huge emotional and monetary burden on patients, so preventive strategies will be a cost-effective means of reducing this burden. Primordial prevention (i.e., intervention prior to onset of disease risk factors) should be implemented by the government, along with the food industry, to educate the public regarding the importance of a healthy diet and adherence to it. Primary prevention should focus on halting the onset of AF in targeted populations who carry risk factors for development of AF. The strategy at the secondary-prevention level includes optimal control of rate or rhythm either by anti-arrhythmic drugs or catheter ablation. Every effort should be made to reduce the incidence of ischaemic stroke by using optimal oral anticoagulation, devices or surgical closure of left atrial appendage. Tertiary level prevention should focus on the management of complications incurred as a result of AF, such as ischaemic stroke, heart failure or asymptomatic left ventricular dysfunction. Since management of AF demands a huge economic burden and the line between thrombotic complications and bleeding complications is a thin one; over-diagnosis and overtreatment of AF should be avoided. The ultimate aim of quinary prevention is to sensitise the physician to follow evidence-based medicine and to get rid of populated myth. This current review summarises a stepwise preventive strategy for AF from the primordial level to the quinary level.
You can read the full article in the latest exciting issue of European Journal of Arrhythmia & Electrophysiology – Volume 5 Issue 2 by clicking here.
Image: Pixabay.com

Jan 5, 2020
You can access and download the SAFE Annual Report by clicking on this button below
SAFE Annual Report 2019
In addition, please see below the message of the President of SAFE, Jon Barrick:
This has been a busy and exciting year for our organisation, especially in terms of advocating on pan-European level. We have continued work around the Stroke Action Plan for Europe, forming an implementation committee with the European Stroke Organisation. We held a seminal event at the EU Parliament raising the profile of stroke more than ever before, engaging with the Deputy Director General of the EU’s DG Sante and the EU Committee of the Regions. Through our funding of Oxford University’s project on the economic impact of stroke, we have produced up to date and compelling evidence about the cost of stroke in Europe. With all this accomplished, we continue to press ahead, as we have now completed the third and final year of the research which will provide us with vital European and country specific data on the future economic impact of stroke and power of interventions. The Economic Impact of Stroke in Europe report will be launched in full at the Joint World Stroke Organisation/European Stroke Organisation conference in Vienna in May 2020.
We have continued with the Angels project to produce vital information booklets on stroke to distribute to patients and families while in hospital. We have provided this information in 15 different languages to ensure that more people across Europe can use our materials to improve the lives of stroke survivors.
We continue our educational work with those who wish to understand stroke support organisations and become advocates for better care through our online teaching and learning tool SSOFT, and our regional and working conferences. A particular highlight for me in 2019 was the concrete evidence of the value of our partnership orientation, our Industry partners have been very supportive again, our outreach to ESO has been reciprocated, and we continue to see the number of SSO’s grow, and then become members of SAFE. Yet again we go into a new year with record membership which bodes well for the future.
As SAFE goes from strength to strength in activities to reduce the number and effects of strokes, the Board must also ensure the long-term sustainability of SAFE. The Board has achieved much of its work through dedicated voluntary time but has recognised that this needs to be added to by full
time paid staff. The Board agreed that SAFE required more permanent leadership to drive forward and to achieve our goals. I am delighted to let you know that we recruited our first Director General this year and I know you will all join me in welcoming Arlene Wilkie into the SAFE family.
In 2019, we have been able to deliver many significant achievements because of our close working community. I would like to thank those that have worked with and for SAFE this year, and to the members and sponsors who have supported us practically and financially. This next year is my last as President and I am looking forward to ensuring we have a solid 2020 of achievement to strengthen the long-term sustainability of all stroke support organisations in Europe.
Jon Barrick
SAFE President

Dec 31, 2019
First published on ScienceDaily.com
In an article in Brain, researchers at the Medical University of South Carolina (MUSC) and elsewhere report which brain regions must be intact in stroke survivors with aphasia if they are to perform well in a speech entrainment session, successfully following along with another speaker.
Aphasia is the inability to speak, write or understand spoken or written language. One of the main causes of aphasia is stroke, the third leading cause of death in the U.S. About one in three stroke survivors develops aphasia.
Patients with non-fluent aphasia speak in short, halting, telegraphic sentences and have trouble forming their words. However, they often understand language relatively well.
“Speech entrainment is asking the person to repeat in real time what they hear and see, or in other words to copy the speech of another speaker,” said Leonardo Bonilha, M.D., Ph.D., who led the study. Bonilha is the SmartState® Endowed Chair for Brain Imaging and an associate professor in the Department of Neurology at MUSC.
Bonilha and Janina Wilmskoelter, Ph.D., a postdoctoral fellow at MUSC, collaborated closely with Julius Fridriksson, Ph.D., professor in the Arnold School of Public Health at the University of South Carolina and director of the Center for the Study of Aphasia Recovery (C-STAR). Other team members include C-STAR collaborators from Johns Hopkins University and the University of California, Irvine.
Speech therapy can be effective in helping stroke survivors communicate better, but non-fluency is one of the hardest symptoms to treat. Speech entrainment is an experimental approach for non-fluent aphasia in which stroke survivors practice speech production in real time by following along with another speaker.
However, not all patients with non-fluent aphasia can follow along with another speaker, suggesting that they might not benefit from speech entrainment therapy should it one day be approved for use in the clinic. Before this study, researchers did not know why some stroke survivors could follow along with another speaker and others could not.
The multi-institutional team of aphasia researchers studied which brain structures were associated with successful speech entrainment. They found that the left lateral temporal cortex needs to be intact for a stroke survivor to successfully follow along with another speaker.
“Our finding helps us understand better what are the neural mechanisms associated with the ability to have one’s speech entrained,” said Bonilha.
Read the full article here.
Image: Pixabay

Dec 28, 2019
First published on ScienceDaily.com
An advanced Magnetic Resonance Imaging (MRI) brain scan analysis in patients with stroke-related, small vessel disease helped predict problems with thinking, memory and even dementia, according to new research published in Stroke, a journal of the American Stroke Association, a division of the American Heart Association.
When a stroke or other disease damages tiny blood vessels in the brain, the condition is known as small vessel disease. This condition is the most common cause of thinking problems (planning, organizing information and processing speed) and can even lead to dementia. Although early treatment could help patients at risk, no effective test is available to identify them.
This study evaluated the accuracy of a new MRI analysis technique using diffusion tensor imaging (DTI), in predicting thinking problems and dementia related to small vessel disease. A single scan measured the brain in fine detail to reveal damaged areas. By comparing these images to a healthy person’s, researchers were able to classify the brain into areas of healthy versus damaged tissue.
Results showed that participants with the most brain damage were much more likely to develop thinking problems. The analysis also helped predict three-fourths of the dementia cases that occurred during the study.
“We have developed a useful tool for monitoring patients at risk of developing dementia and could target those who need early treatment,” said senior author Rebecca A. Charlton, Ph.D., department of psychology at Goldsmiths, University of London, in the United Kingdom.
The study included 99 patients with small vessel disease caused by ischemic stroke, a type of stroke that blocks the blood vessels deep within the brain. Slightly more than one-third were female, average age 68, and most were Caucasian. All participants were enrolled in the St George’s Cognition and Neuroimaging in Stroke (SCANS) study from 2007 to 2015 in London.
Participants received the MRI scans annually for three years and thinking tests annually for five years. Eighteen participants developed dementia during the study, with an average time to onset of approximately three years and four months.
You can read the full article here.
Image: Pixabay

Dec 26, 2019
First published on ScienceDaily.com
Women are more likely to survive a stroke, but have worse disability and poorer quality of life afterwards compared to men, according to research published in the latest issue of Neurology®, the medical journal of the American Academy of Neurology.
The George Institute for Global Health researchers looked at sex differences in treatment and outcomes in 19,652 individuals who had been part of five international randomised controlled trials to identify how to improve the lives of both men and women after a stroke.
Lead author Dr Cheryl Carcel said that variations in how women were treated in hospital and whether they had been receiving appropriate treatment for their risk factors beforehand may partly explain the differences found in the study.
“While the trials we looked at did not specifically investigate treatments, we found a hint that while women who had a stroke were more likely to be admitted to an acute stroke unit, they were less likely to be intubated, treated for fever or admitted to an intensive care unit compared to men. Admission to an acute stroke unit may play a role in the increased survival seen in women.”
“There was also a hint that women were more likely to be taking blood pressure lowering medication, but less likely to have been prescribed blood thinning, glucose-lowering or lipid-lowering medication prior to their stroke than men. This is similar to other studies in cardiovascular disease but we are planning to look at this more closely in further research.”
Stroke is one of Australia’s biggest killers and a leading cause of disability, with more than 56,000 new and recurrent strokes in 2017. As many as 65 percent of stroke survivors suffer a disability, leading to a need for assistance with daily living activities. Most strokes are ischaemic strokes, occurring due to sudden blockage of a blood vessel in the brain.
“While we know women tend to be older when they have a stroke and are more likely to have key risk factors such as high blood pressure and irregular heart rhythms than men, whether they are treated differently and how that affects their longer term outlook was less certain,” added Dr Carcel.
“It is clear that women and men require different types of support after stroke but physicians may also need to pay more attention to risk factor control in women.”
Dr Carcel added that sex diferences in disease risk, management, and outcome are an increasing focus of research and health services delivery, and the study confirmed stroke is an area that needs to be considered in this context.
“In the trials we considered for our analysis, there was an under-representation of women — just 37 percent women in one trial and 42 percent in another.”
Read the full article here.
Image: Pixabay

Dec 24, 2019
First published on ScienceDaily.com
A new gene therapy turns glial cells — abundant support cells in the brain — into neurons, repairing damage that results from stroke and significantly improving motor function in mice. A paper describing the new therapy, which uses the NeuroD1 gene, appears online in the journal Molecular Therapy. Once further developed, this NeuroD1-based gene therapy could potentially be used to treat stroke, which is a leading cause of disability in the U.S., with 800,000 new stroke patients every year.
“The current treatment for stroke has a narrow time window, typically within a few hours after the occurrence of stroke,” said lead author Yuchen Chen, a postdoctoral fellow at Penn State. “Many patients cannot receive the treatment in time and as a result, often suffer from permanent disability caused by irreversible neuronal loss. There is an urgent need to develop a new therapy to regenerate new neurons and restore lost brain functions among stroke patients.”
The human brain has approximately 86 billion neurons. While mini-strokes can be tolerated, moderate stroke involving the loss of billions of neurons leaves detrimental effects that do not spontaneously recover.
“So, the critical question that is still unanswered in the neuroregeneration field is how can we regenerate billions of new neurons in a patient’s brain after stroke?” said Gong Chen, professor of biology and Verne M. Willaman Chair in Life Sciences at Penn State and leader of the research team. “The biggest obstacle for brain repair is that neurons cannot regenerate themselves. Many clinical trials for stroke have failed over the past several decades, largely because none of them can regenerate enough new neurons to replenish the lost neurons.”
Gong Chen and his team pioneered a new approach to regenerate functional neurons using glial cells, a group of cells surrounding every single neuron in the brain that provide essential support to neurons. Unlike neurons, glial cells can divide and regenerate themselves, especially after brain injury.
“I believe that turning glial cells that are already present in the brain into new neurons is the best way to replenish the lost neurons,” said Gong Chen. “These glial cells are the neighbors of the dead neurons in the brain and are likely to share the same ancestral cellular lineage.”
Gong Chen’s team previously reported that a single genetic neural factor, NeuroD1, could directly convert glial cells into functional neurons inside mouse brains with Alzheimer’s disease, but the total number of neurons generated was limited. The research team believed that this limited regeneration was due to the retroviral system used to deliver NeuroD1 to the brain. In the current study, the research team used the AAV viral system, which is now the first choice for gene therapy in the nervous system, to deliver NeuroD1 into mouse motor cortex that had suffered from stroke.
Read the full article here.
Image: Pixabay

Dec 20, 2019
First published on ScenceDaily.com
People who take long naps during the day or sleep nine or more hours at night may have an increased risk of stroke, according to a study published in the December 11, 2019, online issue of Neurology®, the medical journal of the American Academy of Neurology.
People who took a regular midday nap lasting more than 90 minutes were 25 percent more likely to later have a stroke than people who took a regular nap lasting from one to 30 minutes. People who took no naps or took naps lasting from 31 minutes to one hour were no more likely to have a stroke than people who took naps lasting from one to 30 minutes.
“More research is needed to understand how taking long naps and sleeping longer hours at night may be tied to an increased risk of stroke, but previous studies have shown that long nappers and sleepers have unfavorable changes in their cholesterol levels and increased waist circumferences, both of which are risk factors for stroke,” said study author Xiaomin Zhang, MD, PhD, of Huazhong University of Science and Technology in Wuhan, China. “In addition, long napping and sleeping may suggest an overall inactive lifestyle, which is also related to increased risk of stroke.”
The study involved 31,750 people in China with an average age of 62. The people did not have any history of stroke or other major health problems at the start of the study. They were followed for an average of six years. During that time, there were 1,557 stroke cases.
The people were asked questions about their sleep and napping habits. Midday napping is common in China, Zhang said. Eight percent of the people took naps lasting more than 90 minutes. And 24 percent said they slept nine or more hours per night.
The study found that people who sleep nine or more hours per night are 23 percent more likely to later have a stroke than people who sleep seven to less than eight hours per night. People who sleep less than seven hours per night or between eight and less than nine hours per night were no more likely to have a stroke than those who slept from seven to less than eight hours per night.
The results were all adjusted for other factors that could affect the risk of stroke. These include high blood pressure, diabetes and smoking.
People who were both long nappers and long sleepers were 85 percent more likely to later have a stroke than people who were moderate sleepers and nappers.
The researchers also asked people about how well they slept. People who said their sleep quality was poor were 29 percent more likely to later have a stroke than people who said their sleep quality was good.
Of the long nappers, 1 percent of cases per person-years later had a stroke, compared to 0.7 percent of cases per person-years of the moderate nappers. The numbers were the same for the long and moderate sleepers, with 1 percent of cases per person-years compared to 0.7 percent of cases per person-years having a stroke.
Read the full article here.
Image: Pixabay


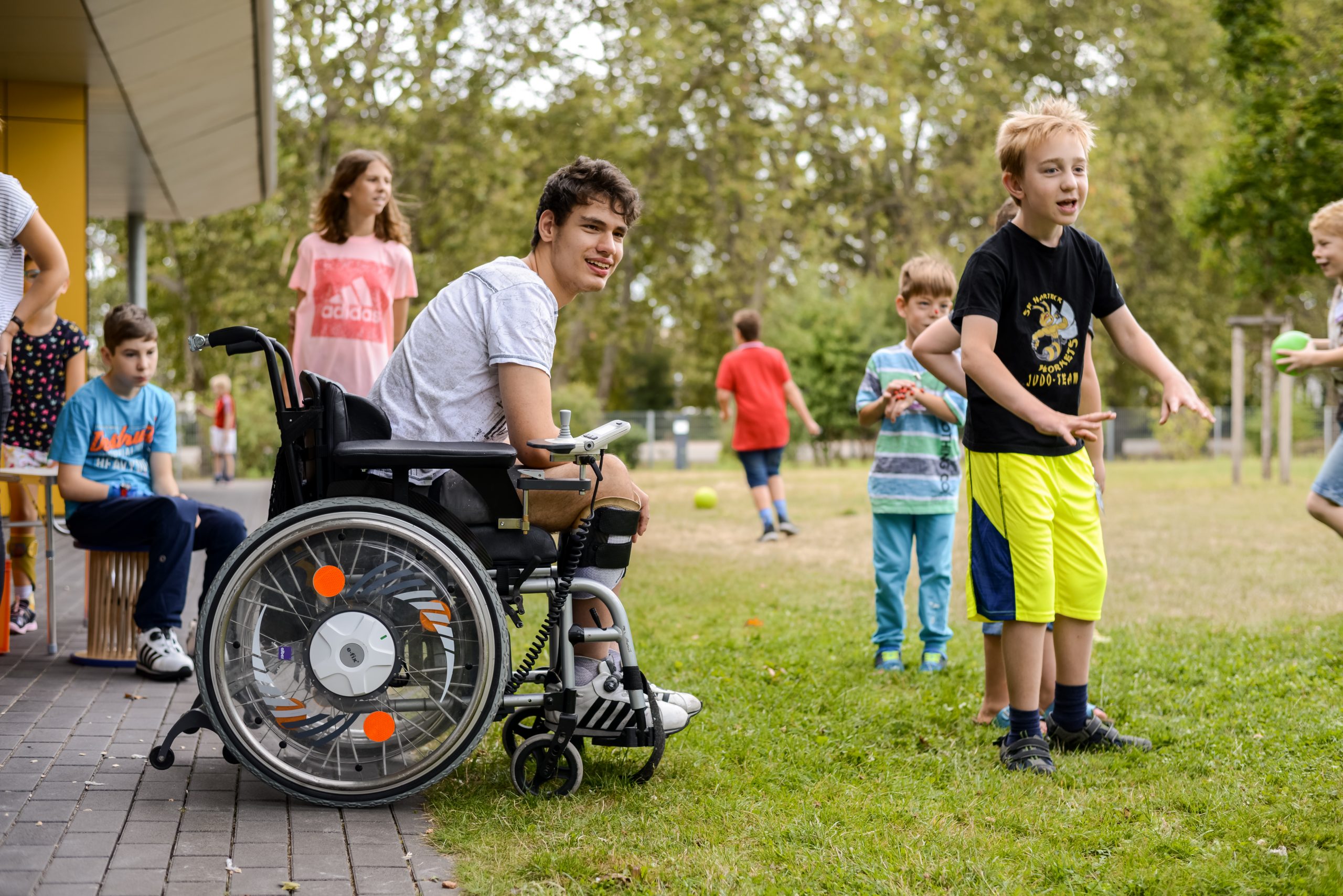 How will my child develop? How will it do in Kindergarten or school? How do we cope with social challenges and which therapies are best with for our child? The diagnosis “stroke” raises many questions – especially when a child is affected. The three day “Summer Camp” offered families with a child affected by stroke an opportunity for an informative and fun-filled weekend. Experts answered questions, psychologists helped developing new perspectives, singer Patricia Kelly gave an exclusive concert and former world-class Wrestler Alexander Leipold offered sport-activities for the children.
How will my child develop? How will it do in Kindergarten or school? How do we cope with social challenges and which therapies are best with for our child? The diagnosis “stroke” raises many questions – especially when a child is affected. The three day “Summer Camp” offered families with a child affected by stroke an opportunity for an informative and fun-filled weekend. Experts answered questions, psychologists helped developing new perspectives, singer Patricia Kelly gave an exclusive concert and former world-class Wrestler Alexander Leipold offered sport-activities for the children. A stroke affects every aspect of life. Young survivors are even in a special situation. They want to return to work, build or maintain relationships and live an independent life – which is not always possible. In a four-day workshop they had the opportunity to talk to psychologists and doctors and to exchange their own experiences. Word-class Mountainbiker Peter Schermann talked about his return into sports after his stroke.
A stroke affects every aspect of life. Young survivors are even in a special situation. They want to return to work, build or maintain relationships and live an independent life – which is not always possible. In a four-day workshop they had the opportunity to talk to psychologists and doctors and to exchange their own experiences. Word-class Mountainbiker Peter Schermann talked about his return into sports after his stroke.
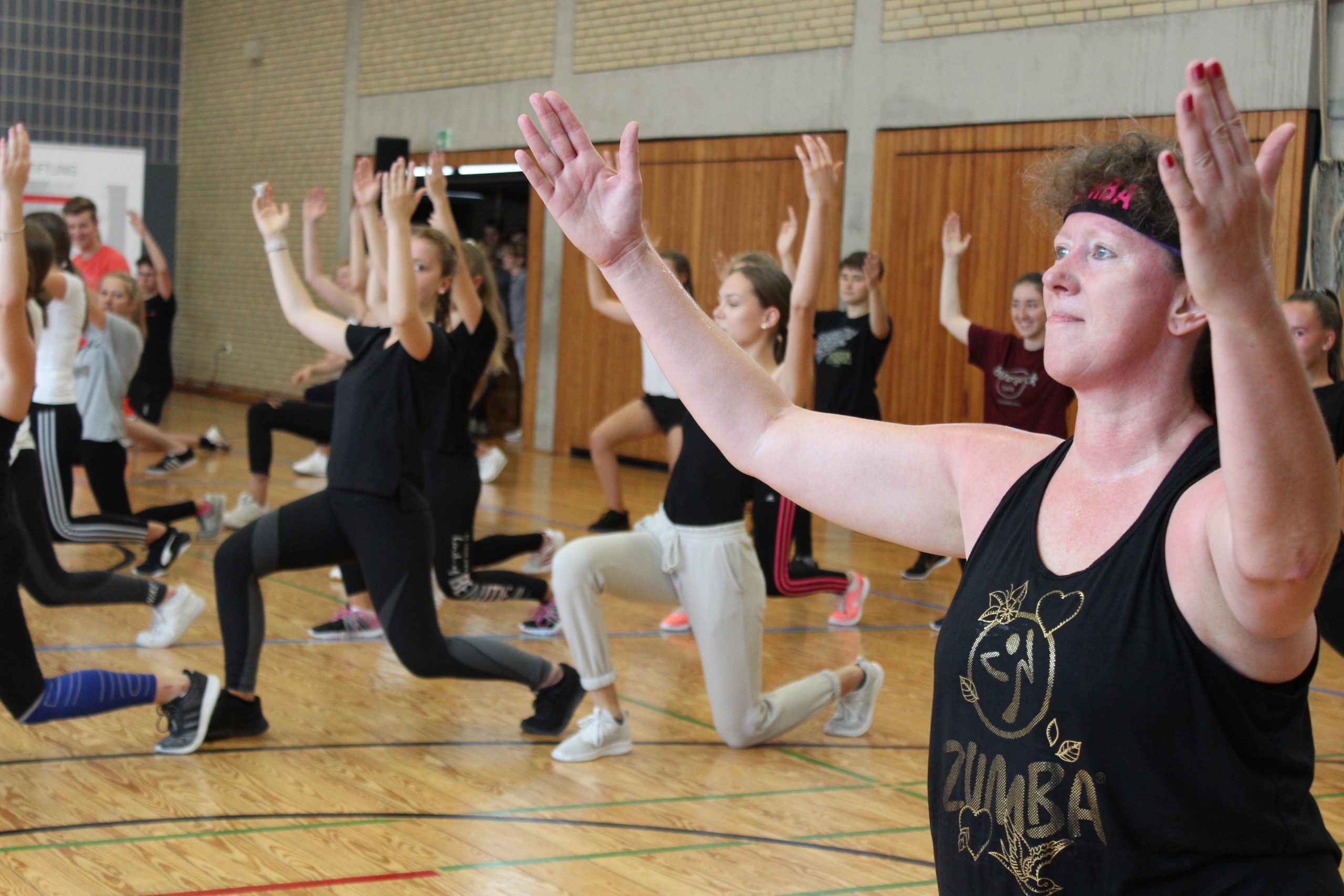


 Not many people know that children can have a stroke. Even experts like podiatrists or therapists often don’t have sufficient information about the topic. The German Stroke Foundation wants to change this by inviting experts to learn more about child stroke. More than 40 doctors and other experts met in Bavaria in 2019.
Not many people know that children can have a stroke. Even experts like podiatrists or therapists often don’t have sufficient information about the topic. The German Stroke Foundation wants to change this by inviting experts to learn more about child stroke. More than 40 doctors and other experts met in Bavaria in 2019.












